Manufacturing News
Common causes of foodborne illnesses identified
Report details most common causes of foodborne illnesses
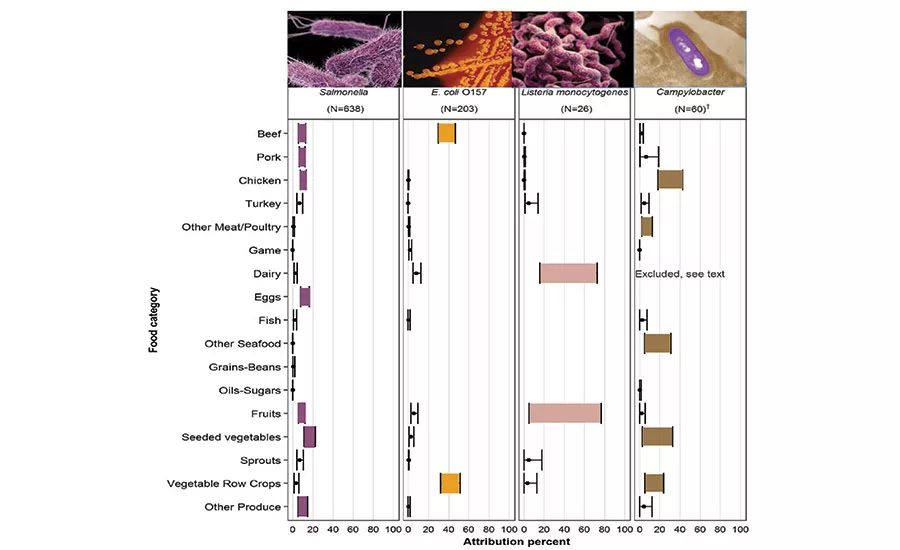
Estimated percentage in the US for 2013 of Salmonella, E. coli O157, Lm and Campylobacter illnesses attributed to 17 food categories, based on a model using outbreak data that gives equal weight to each of the most recent five years of data (2009-2013) and exponentially less weight to earlier years (1998-2008).
†Campylobacter estimates exclude results derived from dairy outbreak data.
The Interagency Food Safety Analytics Collaboration (IFSAC), a joint effort between the USDA, FDA and CDC, has come out with its findings of the causes of foodborne illnesses in 2013. That year, Salmonella illnesses were broadly attributed to a wide variety of foods: E. coli O157 illnesses were most often associated with vegetable row crops (e.g., leafy greens) and beef; Listeria illnesses were most often linked to fruits and dairy products; and non-dairy Campylobacter illnesses were most often attributed to chicken.
IFSAC’s latest study, “Foodborne illness source attribution estimates for 2013 for Salmonella, Escherichia coli O157, Listeria monocytogenes (Lm), and Campylobacter using multi-year outbreak surveillance data, United States,” was compiled with disease data stretching from 1998 through 2013. The latest study was released at the end of December 2017. IFSAC’s study uses data compiled from FDA, USDA and CDC.
Based on a new method first used for 2012, IFSAC developed foodborne source attribution estimates using outbreak data from 1998 through 2013 for four priority pathogens: Salmonella, E. coli O157, Lm and Campylobacter. IFSAC derived the estimates for 2013 using the same method as for 2012 estimates—with some modifications.
The data came from 1,043 foodborne disease outbreaks that occurred from 1998 through 2013. The method relies heavily on the most recent five years of outbreak data (2009-2013). Foods are categorized using a scheme IFSAC created to classify foods into 17 categories that closely align with US food regulatory agencies’ classification needs.
While 2013’s study was based on the approach taken for 2012, one important change was made, and that was related to dairy and Campylobacter.
“Based on outbreaks through 2012, our point estimate was that about 66 percent of foodborne campylobacteriosis was due to dairy products,” says Michael Batz, operations research analyst, FDA.
This result was driven by the fact that the majority of Campylobacter outbreaks in the data were associated with unpasteurized fluid milk.
“We recognized that raw milk is a high-risk product that causes a great number of outbreaks and outbreak illnesses,” adds Batz. “However, raw milk is not widely consumed by the general population. Our goal in this effort is to estimate attribution from outbreaks to non-outbreak illnesses—that is, we want to say something about overall diseases in the population based on outbreaks.”
IFSAC concluded that in this case, the high numbers of raw milk outbreaks likely over-represent the dairy category generally as a source of overall (that is, non-outbreak) campylobacteriosis. This is in line with other foodborne illness studies.
IFSAC identified 2,919 outbreaks that occurred from 1998 through 2013 and that were confirmed or suspected to be caused by the four pathogens covered in this report. Of these, 88 outbreaks with multiple confirmed or suspected etiologies were excluded. Further, IFSAC excluded 1,083 outbreaks with a confirmed or suspected implicated food, 702 outbreaks for which the food vehicle could not be assigned to one of the 17 food categories and three that occurred in a US territory.
The resulting dataset included 1,043 outbreaks in which the confirmed or suspected implicated food or foods could be assigned to a single food category. The numbers include: 638 caused or suspected to be caused by Salmonella, 203 by E. coli O157, 26 by Lm and 176 by Campylobacter.
Estimated Salmonella and Campylobacter illnesses were more widely distributed across food categories than illnesses from E. coli and Lm. Most of the illnesses for the latter two pathogens were attributed to two food categories. For most pathogens, the credibility intervals overlapped to categories with the highest attribution percentages, indicating no statistically significant difference among them.
As noted, Salmonella illnesses spanned multiple food categories. More than 75 percent were attributed to seven food categories, including seeded vegetables (e.g., tomatoes), eggs, chicken, other produce (e.g., nuts), pork, beef and fruits. More than 75 percent of E. coli illnesses were most often linked to vegetable row crops and beef. More than 75 percent of Lm illnesses were most often linked to fruits and dairy products, but the rarity of Lm outbreaks makes these estimates less reliable than those for the other pathogens.
To download the study, visit:
http://tinyurl.com/ycbmlvac.
Looking for a reprint of this article?
From high-res PDFs to custom plaques, order your copy today!




